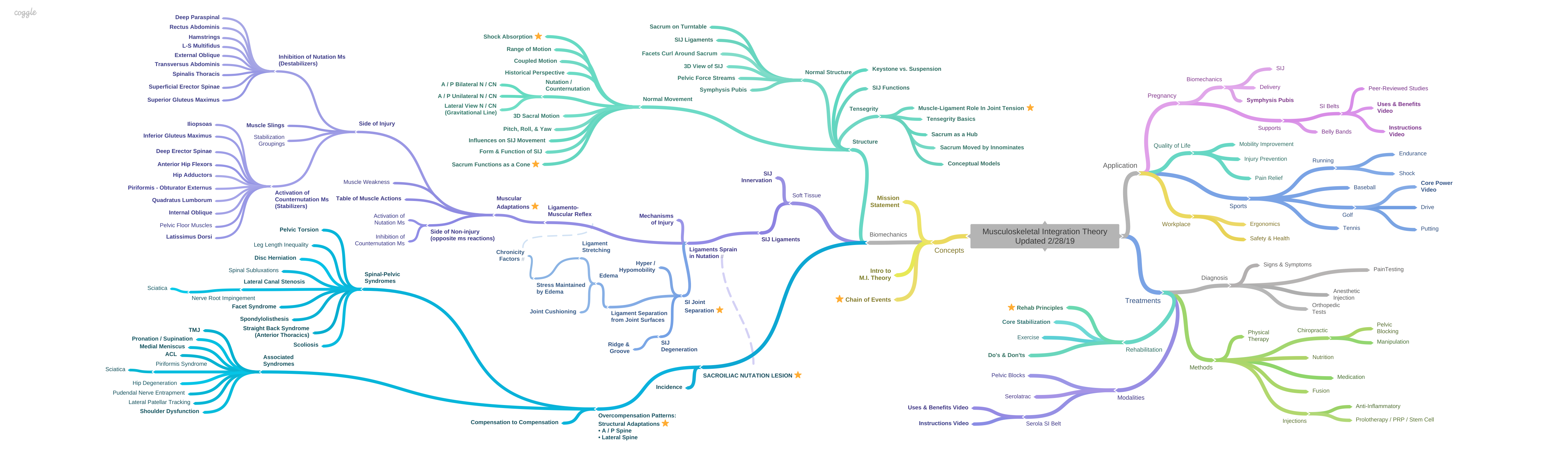
Core Stabilization
Core Power Transfer
In sports and other physical activities, power comes from a stable foundation. Force transfers from the ground, up the legs to the pelvis, through the sacroiliac joint to the sacrum, and then upward through the spine to the arms; each joint functions as a link in this kinetic chain. Smooth and efficient power transfer depends on the integrity of each link. When one link is compromised, the final output power is reduced. In addition to reduced muscular strength and endurance, timing and coordination are impaired.
Power transfer is dependent on smooth synchronization between muscle groups. As one muscle turns off, the next muscle turns on. This timing is dependent on reflexes initiated in the ligaments of the involved joints as they respond to pressure changes during movement. For this reason, ligaments are regulators of muscle tone.
Joint Injury
Joints are held together by ligaments. When ligaments sprain, nerves within them stimulate, or inhibit, certain muscles to keep pressure off the injured ligament. This reaction is known as the ligamento-muscular reflex [1]. (see Ligamento-Muscular Reflex). The functions of the muscles are modified to primarily guard the injured ligament. In other words, the ligaments protect themselves, and use the muscles to do it.
The nervous system must adopt a compensatory program that protects the joint during movement by altering muscle activation patterns and firing sequences. As a result, smooth power transmission will be disrupted, resulting in reduced power, endurance, and coordination.
Because the sacroiliac joint is the center of the body’s shock absorber system, it is the key joint involved in power transference. When we consider that the sacroiliac joint is supported by vast network of ligaments and muscles, it is reasonable to assume that a sprain of the sacroiliac ligaments will cause considerable muscular reaction, even at low levels of stress [2].
My personal research with thousands of individuals, over three decades, has found some degree of sacroiliac sprain in over 99% of the people I tested, as indicated by increased strength with sacroiliac stabilization.
Excess Movement: the Error in Core Stabilization Strategies
It is known that motion in the lumbar spine will be accompanied by motion in the sacroiliac joints [3, 4]. The primary muscles that are active in lumbar stabilization also act as primary stabilizers of the sacroiliac joint [5]p52-59 [6, 7]. For example, the transverse abdominis is of primary importance in stabilizing the lumbar spine by increasing internal abdominal pressure (IAP), and in stabilizing the sacroiliac joint through its attachment to the ilium and spine. Due to confusion about the primacy of the lumbar spine vs. the sacroiliac joint, the core stabilization muscles were thought to create their primary effect on the lumbar spine. However, in the Serola Theory, I am describing the sacroiliac joint as the core structure, not the lumbar spine. In this concept, I demonstrate that the muscular recruitment patterns thought to occur as a reaction to lumbar instability have actually been caused by associated instability in the sacroiliac joint; with this realization, a lot of concepts become clear.
The sacroiliac joints are located where the upper body meets the lower body (see Upper Body meets Lower Body); they are the center of motion and the center of shock absorption, as well as the center of power transfer. As the core, it is supported by a vast number of ligaments and muscles. The interplay between these ligaments and muscles play a key role in sacroiliac movement and stability.
If we look at the sacroiliac joint, we can get a better cause-and-effect relationship between excess movement and muscle inhibition affecting the core muscles. The key is to stabilize the joint and remove stress from the ligaments. This is done by activating the muscles that would stabilize the SI joint and inhibiting the muscles that would destabilize it.
Since load transfer occurs during nutation, most sacroiliac injuries occur in nutation, spraining the nutation resistant ligaments which, in turn, inhibit the nutation inducing muscles and activate the counternutation inducing muscles. The inhibited nutation muscles are the same as those identified as the weak, flaccid, “core” muscles, e.g. the transverse abdominis, multifidus, gluteus maximus, hamstrings, etc. Core stabilization strategies are aimed at strengthening these core muscles. To see examples of the core muscles, please see Nutation Muscles.
Counterintuitive Reasoning
Whether inhibited or contracted, most of the pain in sacroiliac injuries is in the muscles due to lack of circulation, causing a decrease of oxygen and an increase of metabolic toxins. Therefore, activating the muscles gives relief by increasing circulation. So, it is assumed that proper treatment is to exercise the inhibited, flaccid nutation (core) muscles and stretch or relax the tight counternutation muscles. But, strengthening the inhibited muscles and stretching the tight muscles only provide short term relief, while ensuring long lasting pain and dysfunction.
A key to understanding this concept is acknowledging that the muscles that promote nutation are inhibited for a reason; they make the sacroiliac lesion worse by bringing it toward, and even beyond, its normal range of motion in nutation, thereby re-stressing the ligaments that restrict nutation. The counterintuitive aspect is that the popular concept of core stabilization correctly addresses the inhibited nutation muscles with exercises designed to strengthen them but disregards the effects of creating excess nutation at the sacroiliac joint.
Although exercise to the inhibited nutation muscles may result in a significant recovery of size and strength, they will revert to an atrophied state once treatment is stopped and some time passes. If core stabilization treatment is ongoing, it may appear that the patient is progressing because increased circulation will ease the pain and stiffness in the muscles. However, the ligaments will be undergoing continued micro trauma, and the patient will regress once the treatment is stopped.
On the other hand, the counternutation muscles are tight to protect the joint by pulling it away from nutation. But, stretching them will bring the joint towards nutation and will re-stress the sprained ligaments, leading to greater instability. Although the tight counternutation muscles will become stretched and relax, they will tighten again due to the ligamento-muscular response. To see some of the counternutation muscles, please see Counternutation Muscles.
For more, please see The Nutation Lesion and Rehab Principles.
Core Stabilization Exercises and Movement
To my knowledge, the concept of core stabilization began with a book titled Therapeutic Exercise for Spinal Segmental Stabilization in Low Back Pain [5]. In it, Richardson, et al. discussed their findings that certain trunk and pelvic muscles are inhibited and weak in most low back patients. They primarily found that, during exercise and stretching, the motion must be strictly limited or results would be poor. Although Richardson et al. mistakenly considered a movement in the lumbar spine, the Serola Theory states that the nearby sacroiliac joints were the key joints to stabilize.
Regardless of interpretation, their exacting strategies to isometrically strengthen the lumbar and pelvic muscles minimized motion in both the lumbar and sacroiliac spine, so their treatment progressed well. However, it is important to remember, as Richardson et al. [5]p105-155 found, care must be taken to hold the joint within its normal range of motion, then, exercise to the same muscles will provide benefit; however, this is difficult to do and teach due to the patience and focus needed, and resulting slow progress.
As a result, core strengthening has become distorted into just strengthening the inhibited muscles, and then further degraded to just strengthening the trunk and pelvic muscles, with little-to-no regard to controlling movement. One should question the increased prevalence of sacroiliac dysfunction. Are treatments actually providing long term benefits or continued recurrences? Is there increasing awareness or increasing injury, or both?
WHAT TO DO
Conceivably, normal range of motion may be maintained, even during exercise, by use of either a proper sacroiliac belt or during an exacting regimen using an inflatable pressure bladder, as described by Richardson et al. For best immediate results, the Serola Sacroiliac Belt has been designed to normalize the stability and function of the sacroiliac joint during exercise, as well as during daily activities, and thereby normalize power transfer through the core(see the Serola Belt). For best long term results, see Rehab Principles.
References:
- Palmer, I., Pathophysiology of the medial ligament of the knee joint. Acta Chirurgica Scandinavica, 1958. 115(4): p. 312-8.
- Solomonow, M., et al., The ligamento-muscular stabilizing system of the spine. Spine, 1998. 23(23): p. 2552-62.
- Solonen, K.A., The sacroiliac joint in the light of anatomical, roentgenological and clinical studies. Acta Orthopaedica Scandinavica. Supplementum, 1957. 27(Suppl 27): p. 1-127.
- Vleeming, A. The Integrated Function of the Lumbar Spine and Sacroiliac Joint. in Second Interdisciplinary World Congress on Low Back Pain. 1995. San Diego.
- Richardson, C., et al., Therapeutic Exercise for Spinal Segmental Stabilization in Low Back Pain. 1999: Churchill Livingstone.
- Pel, J.J., et al., Biomechanical analysis of reducing sacroiliac joint shear load by optimization of pelvic muscle and ligament forces. Ann Biomed Eng, 2008. 36(3): p. 415-24.
- Snijders, C.J., Transfer of Lumbosacral Load to Iliac Bones and Legs: Part 2 – Loading of the Sacroiliac Joints when Lifting in a Stooped Position. Clinical Biomechanics, 1993b. 8: p. 295-301.