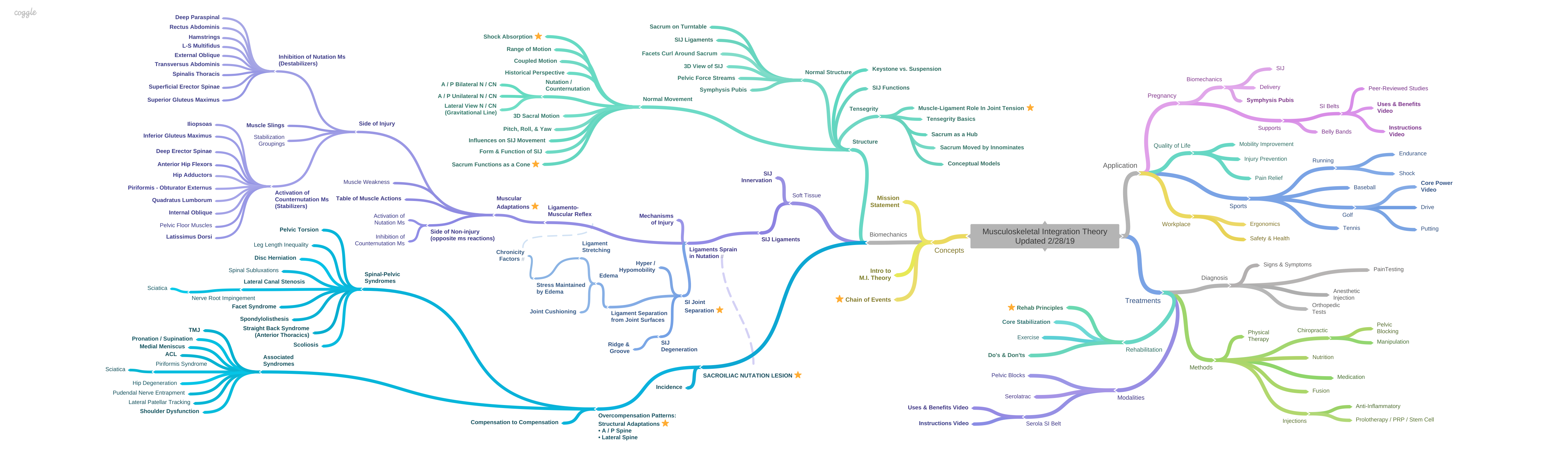
Mechanisms of Injury
The Mechanisms of SIJ Injury
- A fall onto the buttocks
- A motor vehicle accident where the driver brakes hard during impact, or there is a broadside impact which causes twisting
- Stepping into a hole, missing a step, or landing hard on one’s feet
- Repetitive rotation, especially when striking an object, such as in golf, batting, throwing, or soccer, especially when combined with an axial load such as in bowling, ballet, or skating
- Bending, lifting, or twisting
- The cumulative effect of numerous minor stresses to the sacroiliac joint ligaments
- The cumulative effect of nutation pattern injuries in other joints
Axial Force
Basically, any force directed axially from the trunk in an inferior direction will force the sacral base anteriorly, away from the ilia. Likewise, any force directed in a superior direction through the legs will force the ilia posteriorly, away from the sacral base. When the force is greater than the ligaments can withstand, the restraining ligaments will tear, resulting in the Sacroiliac Nutation Lesion.
When force is transmitted superiorly through the legs or inferiorly through the spine a spring like action takes place. As the innominate rotates posteriorly, the sacrum rotates anteriorly. At the sacroiliac joint, this movement (nutation) winds the interosseous ligament, drawing the sacrum and ilium closer [1] [2]p56 [3]p55, but not together [4].Below the sacrum, the feet pronate, the fibulae move inferiorly [5], and the knees twist as the tibia goes farther into internal rotation than the femur. Above the sacrum, the lumbar curve increases like a compressing spring [6]p54&60 as the sacroiliac joint is forced into nutation. Once the energy is absorbed and the end of range of motion is reached, the body reacts by going into counternutation, and all the above actions are reversed as the spring rebounds. Through this mechanism, the sacroiliac ligaments can be seen as the central spring in shock absorption [7] [8] [9]p438.
A destabilizing force can come through the spine, the legs, or the pelvis. Lifting a heavy object puts force on the sacrum in an anterior and inferior direction, inducing nutation. Movements such as a fall, stepping into a hole, a sudden landing on one’s feet, or hard braking in an automobile will transfer force up through the legs, forcing the innominate farther posterior and inferior [10] into nutation.
Bending forward will have a significant effect on the stability of the sacroiliac joint [11]. As one bends, the gravitational line shifts from its normal position posterior to its pivot point of the innominates, the femoral heads, to a position anterior to the pivot. Gravity then forces the innominates to rotate anteriorly. Additionally, as body weight moves anteriorly, the sacral base moves farther from the gravitational line in the horizontal plane, increasing leveraged force on the sacroiliac ligaments. In turn, considerable stress is placed on the hamstrings, abdominals, and other hip extensor muscles, as they try to restrict further anterior rotation of the innominates against gravity, and the muscles may strain and tear. As the muscles attempt to pull the innominates posteriorly against gravity, and body weight forces the sacrum anteriorly into nutation, the ligaments that restrict nutation may sprain as well.
Sacroiliac Joint vs. Lumbar Disc
Bowen & Cassidy [12] found that the sacroiliac joint is 20 times more vulnerable to axial compression and 2 times more vulnerable to axial torsion than the lumbar spine. However, it is able to withstand medially directed force 6 times better than the lumbar spine.
Miller et al. [13] compared the stiffness of the sacroiliac joint to the lumbar disc. They applied forces in several directions and found that, when compared to the disc, the sacroiliac joint can only withstand 5% of the axially directed force, and only 64% of rotation, but it can withstand 624% of a medially directed force, and 700% of force in lateral bending.
The above comparisons explain that the sacroiliac joint is particularly vulnerable to the combined forces of bending, lifting, and twisting but is much stronger than the lumbar disc to horizontal forces and in lateral bending.
Fortin [10] suggests that repetitive impact loading, such as in jumping and landing on one leg, as in ballet or figure-skating, may cause considerable destabilizing shear forces on the sacroiliac joint. Shear forces combined with rotation, as in bowling, golf, and tennis may magnify the injury.
Chronic nutation pattern stress creates micro tears, eventually overloading the sacroiliac ligaments’ ability to maintain integrity. Such stress can come from a nutation pattern lesion other than the sacroiliac joint itself, or insufficient functioning of the body’s shock absorbing system; for example, lumbar hypomobility or foot pronation.
All joints have physiological boundaries; too much or too little motion in almost any joint can be detrimental to the surrounding structure, and the damage may spread to other areas. When understanding the underlying mechanism, it is evident that an injury that causes structural stress anywhere in the body can affect the functioning of the entire musculoskeletal system.
Chou et al. [14] did a study with injection-confirmed sacroiliac joint pain and found that, of 54 patients, “24 (44%) had had a traumatic event (13 motor vehicle accidents, six falls onto the buttock, three immediately postpartum, one severe football tackle, and one pelvis fracture). Eleven (21%) patients were considered to have a cumulative injury (four lifting, two running, three altered gait due to lower extremity disorder, one crew training injury, and one forceful hip extension injury). Nineteen (35%) patients had spontaneous or idiopathic onset of sacroiliac joint pain.”
In a review that included Chou’s article, Cohen [15] stated that predisposing risk factors include “true and apparent leg length deficiency, gait abnormalities, prolonged vigorous exercise, scoliosis, and spinal fusion to the sacrum.” Cohen added that resulting structural damage may include “capsular or synovial disruption, capsular and ligamentous tension, hypomobility or hypermobility, extraneous compression or shearing forces, abnormal joint mechanics, microfractures or macrofractures, chondromalacia, soft tissue injury, and inflammation.”
Jungmann & McClure [16]p5 state that the movement caused by gravity (nutation) becomes greater during pregnancy when the ligaments, which normally resist excessive rotation of the sacrum and ilia, become softened in preparation for birth. They also state that “The range of rotation is further increased if the ligaments become over-stretched and torn through excessive chronic pull of the body’s weight.” However, rather than ascribing this condition to an injury, they suggest it is the part of the natural aging process, which indicates its pervasiveness in the population. They describe a postural index, defined on x-rays, which demonstrates that, as one ages, the effects of gravity cause an increased separation of the sacrum and ilium, as we would see in the nutation lesion. They state that “The common characteristic properties of the chronic-progressive conditions, namely, ‘chronicity’ and ‘progressiveness’ are due to the facts that gravity works perpetually.”
References
- Solonen, K.A., The sacroiliac joint in the light of anatomical, roentgenological and clinical studies. Acta Orthopaedica Scandinavica. Supplementum, 1957. 27(Suppl 27): p. 1-127.
- Kapandji, I.A., The Physiology of the Joints. Vol. 3. 1977: Churchill Livingstone.
- Vleeming, A., et al., The role of the sacroiliac joints in coupling between spine, pelvis, legs and arms., in Movement, Stability, and Low Back Pain, A. Vleeming, et al., Editors. 1997, Churchill Livingstone. p. 53-71.
- Vukicevic, S., et al., Holographic analysis of the human pelvis. Spine, 1991. 16(2): p. 209-14.
- Weinert, C.R., Jr., J.H. McMaster, and R.J. Ferguson, Dynamic function of the human fibula. The American Journal of Anatomy, 1973. 138(2): p. 145-9.
- Vleeming, A., et al., eds. Movement, Stability, & Low Back Pain. 1997, Churchill Livingstone.
- Wilder, D.G., M.H. Pope, and J.W. Frymoyer, The functional topography of the sacroiliac joint. Spine, 1980. 5(6): p. 575-9.
- Grieve, E.F., Mechanical dysfunction of the sacro-iliac joint. International Rehabilitation Medicine, 1983. 5(1): p. 46-52.
- Haldeman, S., et al., eds. Principles and Practice of Chiropractic. 3rd ed. 2005, McGraw-Hill.
- Fortin, J.D. Sacroiliac Joint Dysfunction: Biomechanics, Diagonis, and Rehabilitation. in First Interdisciplinary World Congress on Low Back Pain and its Relation to the Sacroiliac Joint. 1992. San Diego.
- DonTigny, R.L., Evalutation, manipulation, and management of the anterior dysfunction of the sacroiliac joint. The D.O., 1973. 14(1).
- Bowen, V. and J.D. Cassidy, Macroscopic and microscopic anatomy of the sacroiliac joint from embryonic life until the eighth decade. Spine, 1981. 6(6): p. 620-8.
- Miller, J.A., A.B. Schultz, and G.B. Andersson, Load-displacement behavior of sacroiliac joints. Journal of Orthopaedic Research, 1987. 5(1): p. 92-101.
- Chou, L.H., et al., Inciting events initiating injection-proven sacroiliac joint syndrome. Pain Med, 2004. 5(1): p. 26-32.
- Cohen, S.P., Sacroiliac joint pain: a comprehensive review of anatomy, diagnosis, and treatment. Anesthesia and Analgesia, 2005. 101(5): p. 1440-53.
- Jungmann, M. and C.W. McClure, Backaches, Postural Decline, Aging, and Gravity-Strain. 1963, New York, NY: The Institute for Gravitational Strain Pathology, Inc.